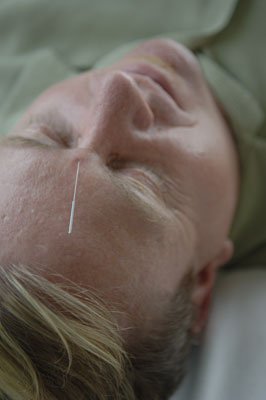
For the last 50 years, the placebo effect has been a dirty word. Real interventions make a physiological change in the body. Placebos do nothing but convince the patient that something is different. Reality states otherwise. Ted Katpchuk, an acupuncturist and Chinese medicine doctor who focuses on the placebo effect in his research, wants to change all that.
Table of Contents
What is a Placebo?
One of the difficult and fundamental questions is what is a placebo? We’ve come to believe a placebo is an inert intervention. A sugar pill.
In most clinical trials of medication, or even with some physical interventions, a group of people with a given condition are given active therapy or medication. The outcomes in this group are compared with a group of people who are given a placebo, but most often are not told which group they are in. Usually both groups improve, even people give the placebo. If the medication is successful, the people on active medication will improve more. The the placebo group improvement is called the placebo effect.
The placebo effect is thought to stem from a belief that a given intervention will help. People convince themselves that the medication is working, and miraculously it does. But the placebo does not change the body physiologically. Or so we thought.
The All Encompassing Placebo
Many of the placebo researchers go further. A placebo is any aspect of a given intervention that may help you feel better, but without a specific physiological interaction with the body. This idea encompasses the whole experience of an individual. The environment of the office, the taste of the pill or tea, and how much the practitioner listens to you. The article even discusses how different colors and shapes of pills have various placebo effects.
A powerful concept in placebo research examines how a given intervention, be it medication, massage, or surgery, is more than simply the intervention itself. For example, my statistics professor at Mount Sinai would often discuss the fact that the clinical trial itself is a placebo. Patients in a clinical trial tend to do better on their medication than the general public. This could be because they feel special, receiving a new medication, being treated by expert doctors with a large staff at their disposal. Then, in the general public, the medications tend to work less well.
Doctor Patient relationship
Kaptchuk would like to explore how best to harness the power of placebos in the healing process. He has focused on the patient doctor interaction as placebo. He even ran a clinical trial of a placebo intervention on IBS where the patients were actually told they were taking a placebo, and that it had clinical efficacy in the past. And amazingly, it worked.
However, this dilemma brings a difficulty with the word placebo. Doctor patient relationship is a skill. A skill that many medical schools have begun to teach, as we loose this skill to technological advances.
Perhaps careful explanation, a caring tone, and an ear to listen can be called a placebo, as it is a non-specific intervention. It is not a chemical pill or an herbal remedy. However, it is also a skill, that can be developed and improved. Kaptchuk would certainly agree with teaching how to wield the healing power of the doctor patient relationship.
Yet, the placebo has a negative tone with the medical establishment, and also much of the population, because we are being fooled into getting better. Perhaps there needs to be a new name for a non-specific intervention.
Placebo: The Social Stigma
What is radical about the placebo idea is that nobody wants to believe that a placebo helps them. And its not just Western medical physicians. Acupuncturists, Chiropractors, and other modalities, as well as patients, fight against the idea that whatever intervention is helping, is a placebo. That means its all in your head.
Kaptchuk and others want to change this stigma. Even if the placebo is all in your head, so what. You feel better. You’re healthier and that’s what counts. But what’s interesting, in some cases, the placebo intervention can actually alter physiology of the body.
A Placebo or Common Sense
A comforting office environment has often be chalked up to placebo. But why would you not want to be comfortable in a doctor’s office with soothing colors and music? It is nerve wrecking enough to go to the doctor. And stress has a real effect on the body. It is just common sense to make the office nice.
I think there is a danger when discussing design of a pill and patient doctor interaction both as placebo because this could reduce the importance of the doctor patient relationship.
Acupuncture itself is an interesting question about the placebo effect. I have a hunch that Kaptchuk believes that acupuncture has a real physiological effect, as he has been involved in many studies comparing acupuncture physiology to placebo physiology, and there is often a difference. But it is not discussed in the article, because the point is that it helps people feel better.
Harnessing the Placebo
The field of studying the placebo itself is young. It questions central tenets to clinical research and shows that our bodies can physically heal ourselves of certain chronic conditions. We do not just react to medication, but also to caring, touch, and the environment.
Like much of good science, these studies bring up more questions than they answer. What is the most important aspect of placebo to focus on. Soft voice, listening to the patient, the examination. Or is it the office lighting, soft colors, and music. As the definition expands, the concept of the placebo can encompass almost anything.
Probably the best way to harness the power of many aspects of the placebo is by not calling it a placebo. Doctor patient relationship, a comforting healing environment, and physical touch are all words that don’t have the placebo stigma. These all help the patient get better, which is what is most important.
Lack of social acceptance in the public and medical community is a challenge that the research will not be able to overcome.