By Hannah & Joe
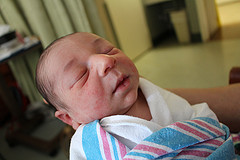
Plans are made to be broken. Knowing this, when anybody asked us if we had a birth plan, one of the staples of contemporary childbirth, we always said we just want him to be healthy. But the truth is we had more plans than we were willing to admit.
It was assumed that we would have a natural childbirth following the traditions of Hannah’s family. When Hannah was six months pregnant, we started a Bradley childbirth classes, which reinforced our assumptions and underlying suspicions of medicalized birth in the United States. These assumptions shaped our decision to give birth with a midwife at a birth center.
Our birth class challenged many of the ideas and images of pregnancy and childbirth that circulate in popular culture. One of the things we learned in birth class is that most pregnancies are not forty weeks long and that it’s perfectly normal to go a week or two past your due date. Our due date was July 9. Joe had predicted a July 4 baby and was planning the taxi route to the hospital around the holiday traffic. We ended up going to the fireworks on the Hudson River, but no signs of a patriotic labor. July 9 came and went without a whimper or a Braxton Hicks.

On Thursday, July 11, Hannah went to the midwife and was told she was zero percent effaced and no dilation. We knew she could go into labor at any moment, but we also began to wonder whether she would. And to worry that we would not make it into the birth center, which only takes women up to 40 weeks and 6 days.
Trying to speed the process along, we continued our eight-mile morning bike rides—with Joe spotting Hannah along the way in what we called the tour de prego. We had been cycling together throughout most of the pregnancy. These were wonderful moments, with the occasional joke and half-worry that Hannah’s uterus would fall out or the baby’s head would be shmushed due to the bumpy roads. We called them uterine bumps. After week 40, we welcomed the bumps, hoping they might induce labor.
On Saturday, July 13, we went for a three-hour urban hike from Fort Tyron Park at 190th street through Inwood Park to 218th street. It was 90 plus degrees, hot, and humid. Hannah was cranky and hardly took notice of the dramatic views until we reached Inwood Hill Park and its old growth forest—the last remaining in Manhattan. The forest was a calming presence as we walked through the hills. By the time we got home, Hannah was exhausted and went to take a nap. When she woke up, she could feel her belly tightening fairly frequently. Joe kept saying these were Braxton Hicks and perhaps a sign that labor was on its way shortly, but Hannah remained skeptical. We watched a movie and went to sleep. On Sunday morning, Hannah woke up at 6AM with bloody show followed by a few contractions. Finally, she thought, this was it.
Figuring we would be home as labor intensified, we decided to get out in the morning. We went to breakfast at a café near our apartment and read the news that George Zimmerman had been acquitted of Trayvon Martin’s murder. At this moment we could still occupy the mental space of worldly concerns and injustices all around us.
After breakfast, we continued to our regular Sunday farmers market run. Joe shopped while Hannah hung out on Columbia’s campus and labored through a few mild contractions spaced more than ten minutes apart. At this point, no one else could tell she was in labor. When we got home, we ate lunch. Hannah retired to the bedroom and watched David Attenboro Nature documentaries of whales and their babies while Joe nervously cleaned and made sure there were plenty of electrolyte-rich fluids in the house.
The contractions grew closer together over the course of the afternoon. By three o’clock, they were regular and about ten minutes apart. At four o’clock, we called the midwife to let her know that labor had started. Throughout this early stage, we practiced labor techniques to figure out which ones might work best for us.
At five o’clock, knowing we would be inside for a long time, Hannah decided she wanted some fresh air, so we walked up Morningside Drive and sat down on a bench overlooking Morningside Park. Things were getting more serious, but still very calm. We came home after half an hour. We were able to eat a normal dinner, but by this time Hannah was becoming less conversational. Contractions continued to grow closer together and were seven minutes apart by eight o’clock.
During this time, Hannah was trying to acclimate to the feeling of a contraction. Throughout pregnancy, she had been more curious than afraid of labor pain. Women compare the feeling to various other sensations. Some compare it to abdominal menstrual cramps, others to severe back ache, and still others to a six-hour marathon or uphill bike ride. Hannah promised herself she would try to articulate the feeling after she experienced it but as the days go by she too is finding it harder and harder to put the experience to words. When a contraction came on, she felt a throbbing sensation in the bottom of her belly. She welcomed the onset of each one and almost looked forward to the powerful surge that came with it. But by the middle she sometimes regretted the prior welcome just happy to ride out the pulsing feeling as it mellowed. Each contraction was slightly different, some stronger than others and some quite mild. She drew a mental picture of what her body was doing, imagining it opening and opening and then giving way to rest.
She was lying on her side in the classic Bradley pose while Joe coached her through contractions. Contrary to what she had expected, the lower belly ache didn’t go away between contractions. As the hours passed we noticed that the forward leaning poses only made the pain worse. Rising from the bed, going to the toilet (which became increasingly necessary as Joe dutifully kept Hannah hydrated), or any forward leaning position was particularly harrowing.
By Monday morning at 3am, Hannah’s contractions were 5 minutes apart or less. We called the midwife with an update. She asked to speak to Hannah who could not respond during her contraction due to their intensity. The midwife told us to call again at 5:30 and plan to meet her at the Birth Center soon after in order to beat the morning rush hour.
After the call, Hannah’s contractions began to slow down. In the meantime, we went to the living room to try a different environment and get things going again. Hannah tried different positions for sitting and standing. She bounced on the birth ball and Joe gave her acupuncture. The contractions came but not as rigorous as before.
At 5:30 the midwife called again and told us that contractions slowing down signaled a long labor and that Hannah’s body was telling her to rest. So we went back to bed and slept. Before long, the contractions began regularly again and by 7:15 they were 3 minutes apart and very strong.
We called the midwife who said that she would come by our apartment to check out the situation. She arrived about a half hour later. The examination showed that Hannah was now fully effaced but only 1 cm dilated. She encouraged us to see this as progress and again prepared us for a long labor, advising us to rest when cued.
We went back to bed and tried to get some more sleep. Hannah’s contractions came and went over the course of the morning. Sometimes the contractions were 10 minutes apart, sometimes less. Around noon we woke up and tried to eat in order to sustain Hannah’s energy through the long labor. But the contractions were erratic. One surged in mid-bite causing Hannah to spit out her pasta primavera on the coffee table and floor.
The lower abdominal pain worsened. Not sure what to do, we consulted our books and binders from the natural childbirth class. We found a discussion of round ligament pain in the uterus. It sounded very much like what Hannah was experiencing. The book said one way to work with this pain is to lie inclined on your back with knees elevated. This gave Hannah significant relief. One big remaining challenge was the toilet. Eventually, Joe figured out how to support her back while she walked to the bathroom, and when she sat on the toilet, he stood in the shower and held her weight as she leaned back.
Hannah labored throughout the afternoon quietly, lying back on the pillows, while we watched BBC costume dramas based on novels by Anthony Trollope. Joe would stop the video when Hannah’s contractions came on and coached Hannah: “Relax your face, relax your shoulders, relax your belly, breathe into your belly, open up the peanut.” The contractions grew closer together, coming once every three minutes and lasting for a minute. By this point, around 4PM, Hannah had reached a zen-like state, laboring quietly through the contractions, signaling their start by tapping Joe with one finger.
We called the midwife who said she would come by at the end of the office day to check our status. She arrived at 7:15. We were excited and sure that all the work we’d been doing had paid off. Hannah imagined she was at seven centimeters by now. She lay back in bed for the exam. The midwife didn’t speak as she felt Hannah’s cervix. With a serious look on her face, she sighed and gently but soberly informed us that Hannah was only two centimeters dilated. This was not the kind of progress one likes to see by this point, and she was concerned that the baby’s head had still not fully engaged. We could wait to intervene, but there was now worry that something—such as a short cord or a wrapped cord—was barring progress and perhaps stressing the baby. She asked if the baby had moved recently, and Hannah recalled some movement within the last hour. The midwife then recommended going to the hospital to get us on a fetal monitor and to start pitocin, which might coordinate the contractions and engage the baby’s head to speed up dilation. We promptly agreed and headed outside together to hail a taxi. A giddy neighbor saw us in the hallway, but we only said we were heading to the hospital.
Before labor, Hannah had expected that the cab ride to the hospital would be very uncomfortable. And during labor, she worried about the pain of having to lean forward during parts of the ride. But she was surprised at the physical relief she got while leaning backwards in the back seat, with Joe at her side and the midwife in the front. The physical relief, however, was accompanied by a heart heaviness—the fear that the baby she had carried all these months might not be well. All she cared about now was the baby’s health and she even began to wish for an immediate c-section—not to ease the pain but to have the baby born safely.
We arrived at the hospital. The midwife rushed us through triage and we were in a delivery room within a few minutes. There were about five minutes of paperwork done by Joe, the midwife, and the nurses, during which time Hannah was alone in the room wondering what would happen. It felt like an eternity. When the nurse returned, she started an IV and the fetal monitors were hooked up. We heard the sound of the baby’s steady heartbeat and breathed a sigh of relief. The nurse explained that they were going to administer some pitocin shortly and that Hannah could tell her if she wanted an epidural at any time. By this point, Hannah had resolved to get the epidural—hoping, as the midwife had explained, that it would give her time to rest and relax, supporting dilation and giving her the energy to push the baby out.
The anesthesiologist arrived shortly after to administer the epidural. He was jovial and chatty, assuming we had planned an epidural all along without any knowledge that we had been in labor already for over 30 hours. “It’s a beautiful day, and it will be even more beautiful when you have your baby in your arms without a hint of labor pain.” On any other day, Hannah would have considered this man naïve to the problem that his profession poses for pregnant women. But at this moment, his presence was a source of comfort. As he walked her through the procedure and prepared her for the series of sensations, she became increasingly calm, hardly noticing the tube being inserted near her spine—something she would have recoiled at not more than thirty hours ago. With the pleasant tingling moving first down her leg and then through her body, she softened and started to talk—something she hadn’t really done in hours. The senior anesthesiologist was now in the room, and Hannah pleasantly chatted with him about how they had taken childbirth classes and been taught all about the cascade of medical interventions as well as the negative effects on the baby associated with epidurals.
The anesthesiologist responded with the charmed assurance of one whose authority in society is beyond question by those who really matter. “No, this is bogus. The epidural does not have an effect on the baby. The medication does not enter the blood stream and if it would it would be digested within seconds so it could never reach the umbilical cord.”
Hannah responded, “I guess it’s just a clash of cultures.” Silently she reflected on the video about epidurals they had watched in class. In the video, an animated reindeer gives birth with an epidural. She is shown on her back looking rather comatose with a sea of wires coming out of her. The video stresses that the coach does not relax and abandon the birthing mother, but rather continues to support her throughout the epidural and subsequent medical procedures. But it also shows the mother reindeer itching from the medication and calmly warns the parents-to-be that their baby may seem drugged for the first six weeks of his life.
Soon after the epidural was in place and working, at about 9pm, the nurse administered a small dose of pitocin. Hannah lay on her side while everyone watched the monitors. At one point the heartbeat seemed to decelerate so they stopped the pitocin. But upon further observation the nurse noticed that the monitor had moved and the heartbeat was probably fine.
They continued at a low dose of pitocin for about a half an hour and gradually increased it once or twice. As time passed, Hannah could feel a crescendo of pressure and release in her belly. The midwife advised both Joe and Hannah to rest for now and she would check the dilation at 11pm. We sat quietly while Joe tried to calm Hannah who heard variations on the monitor that she interpreted for the worse, although Joe, who could see the numbers, reassured her that everything was fine. Still, Hannah tried to make peace with the real possibility that this labor would end in a c-section.
At 11pm, the midwife returned. She placed her hands near the cervix, smiled, and gently said, “She’s nine centimeters.” This was the best news we could have hoped for and unusually fast progress for a first time mother. The midwife and everyone else concurred that all those hours of labor were indeed doing work and prepared Hannah’s body to respond quickly to the pitocin and maybe even the epidural. Typically, women who go directly on the epidural do not have this experience. “I’ll come back at 11:30 and see if you’re ready to push.” So much time had passed, it was almost hard to believe that the end might be near.
At 11:30, sure enough, Hannah was fully dilated. The midwife flattened the bed to prepare for delivery. Hannah laid on her back with her legs bent. The midwife and Joe stood opposite each other, flanking the left and right side of Hannah’s legs. One foot was supported by Joe’s hip, the other by the midwife’s. We were ready to push.
When the contractions came, Hannah held her legs under her knees and, following the midwife’s directions, took a deep breath, bared down, counted to ten and exhaled, repeating this two more times with the same breath. The baby descended down the birth canal very fast. Hannah felt no pain but could feel the baby’s limbs wiggling way down low and tickling her insides. As the baby’s head came close to crowning, Joe could see his brown hair. The midwife told Hannah to touch his head while still in the birth canal. At this point we could anticipate holding him.

With each push, the midwife swept the perimeter of the vagina in half circle motions gently stretching it. As the baby’s head came closer to emerging, the midwife would pull the head gently towards her, coaxing him out into the world. Twenty-nine minutes after pushing began, Hannah bared down one final time and a crying Samuel Lewis slid out with his right arm extended like the Statue of Liberty. Hannah reached down, picked him up, and laid him on her chest.
Plans are made to be broken. But sometimes broken plans teach you the importance of keeping an open mind. We still believe that birth is overly medicalized in the United States, but we have come to understand that medical interventions have a place even within a “natural birth.” These two worlds are not mutually exclusive and too often treat each other with hostility and distrust.
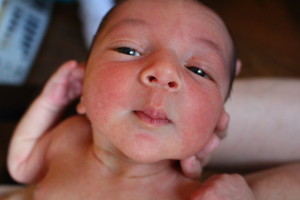
We were lucky to have a midwife who has the understanding, expertise, and attention that, despite what doctors say, makes midwives unique and invaluable. As medical professionals, the best midwives know when and how to use intervention and the best doctors and hospitals trust midwives to make difficult decisions when necessary. Our plans were indeed broken but we are happily surprised to say that it was a positive experience.
Samuel Lewis is a miracle baby who came to us as a welcome surprise after more than ten years together. Now we look forward to new experiences as a family, more plans, more plans that are broken, and more unexpected joys.



